 |
||||||||||
Date: July 19, 2026
by Chaya Venkat

In spite of the many new drugs as well as ever more fancy drug combinations that begin to look like an alphabet soup, to this date the only therapy that has a proven ability to cure CLL is a stem cell transplant from a matched donor. (We are not talking of autologous stem cell transplants, where the patient’s own stem cells are used. Auto stem cell transplants invariably relapse. Very few patients are ultimately cured by this technique.) It is worth our while to keep an eye on developments in the area of allogeneic (donor) stem cell transplants and we review below two very interesting papers to bring you up to speed.
A lot has changed in the past few years, as far as allo stem cell transplants are concerned. A decade ago, the only allo (short for "allogeneic") stem cell transplants done were very heavy-duty affairs. The patient went through very heavy chemotherapy, as well as high dose full body radiation as the preparatory regimen. The idea is to kill each and every cancer cell in the body, and by this process kill all the stem cells and other immune system cells as well. The technical name for this take-no-prisoners approach is “myeloablative”. The preconditioning regimen for a myeloablative transplant was so tough that patients had to meet strict age limit as well as general fitness limit to be eligible for stem cell transplants. You can read more of the details of how stem cell transplants are done in our Primer on Bone Marrow SCTs. Most of the time, the donors were related to the patient, since at that time we did not know enough about matching different HLA types to use unrelated donors (Matching Made Simple).
There are a lot more options now. In addition to related donors, matched but unrelated donor “MUD” transplants are becoming common. We have fine-tuned the requirement of myeloablative transplants. Even more important, we have discovered the way to do “mini” transplants (the formal name for this is non-myeloablative transplant). We have discovered that it is not necessary to go to extreme lengths to kill of each and every cancer cell in the body, at the expense of huge toxicity and death-due-to-therapy. It turns out that once the donated stem cells get established, they can and do generate new immune system cells that are able to go out, hunt and kill the remaining traces of cancer. This is called Graft-versus-leukemia “GVL” effect. It allows us to get away with a much milder preconditioning process, using somewhat lower dose chemotherapy and lower dose radiation. Don’t get me wrong, the preparatory therapy for mini transplants is still pretty potent, but it is not the total thermonuclear war needed for full myeloablative transplants.
The “kinder and gentler” approach used in mini-transplants has made it possible to expand the eligibility criteria to older patients, and those in less than perfect health. This is particularly important for CLL patients, since the majority of CLL patients are diagnosed later in life. Improved understanding of HLA matching and better organized donor banks for stem cells has made it more likely that unrelated donors can be found. We are even exploring the use of cord blood (material that is otherwise discarded after babies are born - see Umbilical Cord Stem Cell Transplants) as a source of stem cells.
All these new options are good news, but at the same time it becomes ever more complex to make therapy choices. What exactly are the survival statistics associated with the new fangled mini-transplants? How do the statistics stack up for related donors versus unrelated donors? The first paper below from the “Hutch” answers these two questions, specifically as they pertain to CLL patients. The second paper below (also from the Hutch) customizes the risk profile for individual patients. These two papers present absolutely top notch research, based on large enough patient cohorts to give meaningful statistics, and details that answer a lot of questions. Both papers are hot of the press, and coming from one of the top rated expert centers for stem cell transplants, the information is very credible.
Until recently, the conventional wisdom was that you are one lucky dude if you had a sibling with perfect HLA match. Even now, it is no small task to find exactly matched unrelated donors, and that is especially true if we are talking about exotic ethnicity. In the first paper from the Hutch, significantly better response statistics are seen for transplants done with matched, unrelated donors “MUDs” than with sibling donors. I admit I was surprised by this result. The abstract of this important paper is given below. Write to us if you want help in locating the full length article. As always, I have tried to summarize below the highlights of the article for your easy reference. But if a mini-transplant is in your immediate future, I strongly urge you to read the full paper. There are lots of details in the paper that I am not able to capture in my thumbnail summary.
Here is how the results played out, for this group of patients:
And that brings us to the million dollar question, how do these statistics play out for the individual patient, how do they pertain to you? It is all very well to look at statistics based on a whole bunch of people, but what if your particular situation is very extreme, you hold down one end of the distribution curve? What if you are a very fit and younger patient, some one who has led a blameless life as far as taking care of your health, and whose only problem is poor prognosis CLL making it necessary for you to consider a stem cell transplant? This paper suggests that poor cytogenetics does not influence the decision. Does that imply your otherwise sterling characteristics are likely to give you much better chance of success compared to the generally older and less healthy patients described above? If you also succeed in locating a perfectly matched MUD donor, can you expect to do better than the 75% 2-year survival rate quoted above? Incidentally, folks who survive a bone marrow transplant for 2 or more years can breathe a sigh of relief, the vast majority of them survive trouble-free and CLL-free in the years to come. I think you can see where I am heading with this. How much higher can we push this almost-cure rate of 75%?
Excellent question, and the answer is given in the second paper we review.
J Clin Oncol. 2026 Jun 1;23(16):3819-29. Epub 2026 Apr 4.
Hematopoietic cell transplantation after nonmyeloablative conditioning for advanced chronic lymphocytic leukemia.
Sorror ML, Maris MB, Sandmaier BM, Storer BE, Stuart MJ, Hegenbart U, Agura E, Chauncey TR, Leis J, Pulsipher M, McSweeney P, Radich JP, Bredeson C, Bruno B, Langston A, Loken MR, Al-Ali H, Blume KG, Storb R, Maloney DG.
Fred Hutchinson Cancer Research Center, 1100 Fairview Avenue N, D1-100, PO Box 19024, Seattle, WA
PURPOSE: Patients with chemotherapy-refractory chronic lymphocytic leukemia (CLL) have a short life expectancy. The aim of this study was to analyze the outcome of patients with advanced CLL when treated with nonmyeloablative conditioning and hematopoietic cell transplantation (HCT).
PATIENTS AND METHODS: Sixty-four patients diagnosed with advanced CLL were treated with nonmyeloablative conditioning (2 Gy total-body irradiation with [n = 53] or without [n = 11] fludarabine) and HCT from related (n = 44) or unrelated (n = 20) donors. An adapted form of the Charlson comorbidity index was used to assess pretransplantation comorbidities.
RESULTS: Sixty-one of 64 patients had sustained engraftment, whereas three patients rejected their grafts. The incidences of grades 2, 3, and 4 acute and chronic graft-versus-host disease were 39%, 14%, 2%, and 50%, respectively. Three patients who underwent transplantation in complete remission (CR) remained in CR. The overall response rate among 61 patients with measurable disease was 67% (50% CR), whereas 5% had stable disease. All patients with morphologic CR who were tested by polymerase chain reaction (n = 11) achieved negative molecular results, and one of these patients subsequently experienced disease relapse. The 2-year incidence of relapse/progression was 26%, whereas the 2-year relapse and nonrelapse mortalities were 18% and 22%, respectively. Two-year rates of overall and disease-free survivals were 60% and 52%, respectively. Unrelated HCT resulted in higher CR and lower relapse rates than related HCT, suggesting more effective graft-versus-leukemia activity.
CONCLUSION: CLL is susceptible to graft-versus-leukemia effects, and allogeneic HCT after nonmyeloablative conditioning might prolong median survival for patients with advanced CLL.
PMID: 15809448
_____________
OK, now we have a better fix on how full blown myeloablative transplants compare with non-myeloablative "mini" transplants, and how sibling donor transplants compare with matched but unrelated donor “MUD” transplants. But that still does not give us a fix on the prognosis of individual patients.
A few months ago I spent two hours on the phone with one of our top stem cell transplant experts. One of the points I took away from our conversation is that general statistics based on across the board patient populations do not begin to describe the risk (or lack of risk!) where individual patients are concerned. Most of the papers do not address this issue. My contact told me there is a world of difference in the results one can expect in patients that are otherwise in good general health, who go into a stem cell transplant in fighting trim, and those that are handicapped by a host of other health problems.
Makes sense to me. Whether it is a matched donor or MUD, stem cell transplant is serious business. Heavy duty chemo and radiation to do a real number on the immune system you are born with. For patients in fragile health to begin with, this can be the most difficult hurdle. Next step is replacing it with one obtained from a generous donor, and then keeping your fingers crossed the foreign stem cells will find their new home to their liking. Engraftment of the new stem cells is only the beginning of the process, they must then be able to root out and kill any remaining traces of the CLL (graft-versus-leukemia “GVL” effect) and do it before the cancer has a chance to grow back. And they must not do too much damage to the rest of your body in the process (acute Graft Versus Host Disease “GVHD”). Last but not least, it is hoped that all this happens reasonably quickly, keeping the window of vulnerability small for opportunistic infections, second cancers, failure of major organs etc. None of this is easy, and it makes sense that your body can better tolerate the rigorous process if you are not carrying a lot of excess baggage in terms of other health complications.
This is where the next article I am going to review is a gold mine of information. This too is from the Hutch, which seems to specialize in stem cell transplants. This article too is hot off the press, about as up to date as you can get. The abstract is given below. Write to us if you want to read the full text and would like our help in locating it, but I must warn you it is heavy reading, full of statistical and medical jargon. I read it, cover to cover, and pulled together a cheat-sheet for you folks who may not be into masochism as much as I am. But I will be the first one to admit, nothing like going to the source to get the full flavor.
| Comorbidities | Definitions | Penalty Points |
| Arrythmia | Atrial fibrillation or flutter, sick sinus syndrome, and ventricular arrhythmias |
1 |
| Cardiac | Coronary artery disease, congestive heart failure, myocardial infarction |
1 |
| Gastrointestinal | Crohn’s disease, ulcerative colitis | 1 |
| Diabetes | Requiring treatment with insulin or oral hypoglycemics, but not diet alone |
1 |
| Cerebrovascular Disease |
Transient ischemic attack or cerebrovascular accident |
1 |
| Psychiatric | Depression/anxiety requiring psychiatric consult or treatment |
1 |
| Hepatic - mild | Chronic hepatitis, Bilirubin between 1-1.5 times of normal upper limit, or AST/ALT between 1-2.5 times of normal upper limit |
1 |
| Obesity | Patients with a body mass index more than 35 kg/m2 |
1 |
| Infection | Requiring continuation of anti-microbial treatment after first day |
1 |
| Rheumatologic | Lupus, RA, polymyositis, mixed CTD, polymyalgia rheumatica |
2 |
| Peptic Ulcer | Requiring treatment | 2 |
| Moderate/severe Kidney Problems |
Serum creatinine more than 2 mg/dl, on dialysis, or prior kidney transplantation |
2 |
| Moderate Pulmonary Disease |
difficulty breathing on slight activity | 2 |
| Prior Solid Tumor | Treated at any time point in the patient’s past history, excluding non-melanoma skin cancer |
3 |
| Heart Valve Disease | Except mitral valve prolapse | 3 |
| Severe Pulmonary Disease |
Difficulty breathing at rest or needing oxygen | 3 |
| Moderate/severe Liver Problems |
Liver cirrhosis, bilirubin more than 1.5 times of upper normal limit, or AST/ALT more than 2.5 times of upper normal limit |
3 |
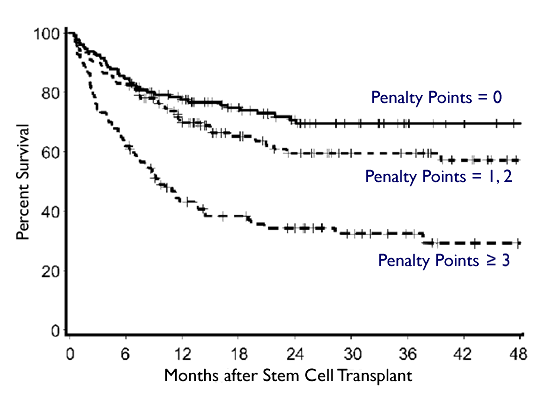
Comorbidity Index and Post-transplant Survival
Sorror, et al.
Blood. 2026 Jun 30; [Epub ahead of print]
Hematopoietic cell transplantation-specific comorbidity index: a new tool for risk assessment before allogeneic HCT.
Sorror ML, Maris MB, Storb R, Baron F, Sandmaier BM, Maloney DG, Storer B.
Fred Hutchinson Cancer Research Center, Seattle, WA
We previously reported that the Charlson Comorbidity Index (CCI) was useful for predicting outcomes in patients undergoing allogeneic hematopoietic cell transplantation (HCT). However, the sample size of patients with scores of >/=1, captured by the CCI, did not exceed 35%. Further, some comorbidities were rarely found among patients given HCT. Therefore, the current study was designed to a) better define previously identified comorbidities utilizing pretransplant laboratory data, b) investigate additional HCT-related comorbidities, and c) establish comorbidity scores that were suited for HCT. Data were collected from 1055 patients, and then randomly divided into training and validation sets. Weights were assigned to individual comorbidities according to their prognostic significance in Cox proportional hazard models. The new index was then validated. The new index proved to be more sensitive than the CCI since it captured 62% of patients with scores >0 compared to 13%, respectively. Further, the new index showed better survival prediction (likelihood ratio of 23.7 versus 7.1 and c statistics of 0.661 versus 0.561, P=< 0.0001, respectively). In conclusion, the new simple index provided valid and reliable scoring of pretransplant comorbidities that predicted non-relapse mortality and survival. This index will be useful for clinical trials and patient counseling before HCT.
PMID: 15994282
____________
The first paper we reviewed above provides very timely and eye-opener statistics comparing related donor transplants to MUDs. Rejoice, all ye with no brothers or sisters that match! You too have a fighting chance, if you can find a well matched MUD. Get the word out in your community, get people to volunteer as stem cell donors. The larger the pool of volunteers in the stem cell bank, the better your chances of finding a good MUD.
In addition to its value as a research tool, the second paper has huge implications from your individual perspective as you ponder therapy choices. If you are unfortunate enough to have a high number of penalty points against you going in, it might be worth taking a second look at your other options, discussing your chances of surviving the transplant procedure with your doctors. On the other side of the coin, if you are in general good health except for the CLL, and you are fortunate in having a well matched donor, stem cell transplant with its ability to actually cure the CLL starts looking a whole lot better. I would not be surprised if this model or a variation of it becomes the standard for setting eligibility criteria for mini stem cell transplants.
Let’s see: the first paper, devoted exclusively to CLL patients, says the median 2-year survival for MUD transplants is 75%. The second paper says the bonus for going in with zero penalty points is quite a bit, some where in the region of 5-10% higher survival rates, compared to the average guy with 1-2 penalty points. Dare we hope, that increases the 2-year survival rate for well matched MUD transplant in healthy CLL patients to the 80-85% range? Remember, the two year survival rate is pretty close to an almost-cure, the large majority of patients who make it up to that point go on to live normal lives. You can see that in the graph above - see how the survival curves flatten out after 24 months? Keep your fingers crossed folks. Mini transplants with well matched MUDs are looking pretty good, and likely to get better as we learn better ways of doing them.
I agree, not every health complication is under your control. But the other side of the coin is also true, there are some things you can do to improve your penalty point score. We have discussed many of these lifestyle changes before, but they are worth repeating in this context. Pulmonary inflammation is something that should be at the top of every CLL patient’s watch list (Role of Pulmonary Inflammation in CLL; CLL Chronic Inflammation and What You Can Do About It). If you continue to smoke even after getting diagnosed with CLL, you probably need to have your head examined as well. Remember, psychological problems carry a penalty point too. A glass of red wine is good for you (resveratrol in red wine helps killing of cancer cells), but heavy drinking is bad for your liver any way you look at it. Staying well hydrated by drinking lots of water is an excellent way of protecting your liver and kidneys. Obesity is a health risk in surviving transplants, it is also a health risk in just about every other aspect of living. Regular and vigorous exercise does wonders for your heart and general cardiovascular system, but did you know it is also an excellent way of keeping down systemic inflammation? Watch out for “poly pharmacy”, fist full of pills swallowed without due consideration for their interactions with each other and potential for significant liver toxicity. This is equally true whether the pills are ‘drugs’ or ‘herbal supplements’. For crying out loud, herbs are drugs!! They don’t become any safer just because some Oriental Cancer Guru recommended them on the Internet, for a modest fee. On the other hand, you might want to consider adding well researched supplements such as fish oil, and green tea extract EGCG to your daily diet, after discussing them with your doctor.
There are no guarantees in life, except that each and every one of us will die some day. But each of the things suggested above will have a positive impact on your health, slowly but surely. If you had pancreatic cancer or one of the other cancers with a short fuse, there is no time to for lifestyle modifications to kick in with their beneficial results, you barely have enough time to make your hail-Mary therapy choices. But CLL is an indolent disease, even the most aggressive versions give us months of lead time. This means most of us do have the luxury of time to read, learn, and implement the lessons learned. “The life you save will be your own,” should be the mantra you repeat to yourself, every single day.
 Enter Keywords: |
———
Disclaimer: The content of this website is intended for information only and is NOT meant to be medical advice. Please be sure to consult and follow the advice of your doctors on all medical matters.
Copyright Notice:
Copyright © 2026-2007 CLL Topics, Inc. All Rights Reserved.
All materials contained on this site are protected by United States copyright law and may not be reproduced, distributed, transmitted, displayed, published or broadcast without the prior written permission of CLL Topics, Inc. You may not alter or remove any trademark, copyright or other notice from copies of the content.
However, you may download and print material from CLLTopics.org exclusively for your personal, noncommercial use.
———
