 |
||||||||||
Date: January 5, 2026
by Chaya Venkat
Related Articles:

If you have been around the CLL scene for a while, and especially if you have been reading review articles on our website, you are familiar with response statistics quoted for the various chemotherapy and immunotherapy combinations. Just as in baseball, researchers and patients keep track of statistics such as “overall response”, “complete response”, “partial response” etc. Some of the more recent combo therapies such as FRC (fludarabine, cyclophosphamide, Rituxan) and RF (Rituxan, fludarabine) have become famous for the high percentage of patients who respond to them. For a group of chemo naïve patients, it is not unusual to see overall response rates over 90%, with a substantial fraction of these responders getting the coveted “CR” or complete response.
Of course, by now we also know that a “complete response” does not mean one is cured. Far from it. Most (if not all) patients who get a CR response will inevitably relapse, sooner or later. Aha! That is the crucial phrase, “sooner or later”. I don’t know about you, but I would much prefer to relapse “later” than “sooner”, thank you. I would also like to live longer, free of CLL, as a result of undergoing the therapy. This brings us to two more statistics that are much less frequently reported: “overall survival (OS)” and “progression free survival (PFS)”. For a change, the phrases mean exactly what they say. OS measures the percentage of patients who are alive after a given period of time, and PFS measures the percentage of people who are alive and free of CLL over a given period of time.
It is obvious these are the two statistics that matter most to patients, much more so than the percentage of CRs and PRs. Why then are they so rarely reported? The answer is dollars and time. It is far easier to come up with response statistics such as the overall response rate or the percentage of CRs achieved immediately after completion of the therapy. But in order to monitor overall survival or progression free survival, the patient cohort has to be monitored for a long period of time, most often for several years, and this becomes expensive. CLL is an indolent cancer. Survival is measured in years (even decades, for the lucky “smoldering” group). Measuring and showing improvement in the short fuse cancers is a lot easier than it is in CLL.
Another aspect of CLL clinical trial results that leaves me dissatisfied most of the time is that they do not distinguish between different risk categories of patients. Just about all the CLL experts now agree that cytogenetic abnormalities (FISH test results) and IgVH gene mutation status play an important role in defining the risk category of patients. Does getting a CR mean the same thing for patients in different risk groups?
Let me put it in blunt terms. If you are a “Bucket C” patient with p53 deletion and you got a CR after a particular therapy, will you live as long as a “Bucket A” patient who started with a more benign 13q deletion and who also got a CR? (For our “Bucket” definitions of risk categories, read What Type of CLL Do You Have?) Are these two CRs equivalent, of the same value to the two patients? This is where the rubber meets the road! Frankly, I do not care a fig for these rather artificial definitions of “complete responses” and “overall responses”. As a patient spouse, what matters to me is information that allows me to judge whether or not guys like my husband, with his given FISH status and IgVH status are likely to live longer, and be free of this disease for longer periods of time as the result of a given therapy. I am sure you will agree, it is cold comfort to get a CR, only to have it relapse quickly, or die soon after! A rose by any other name smells just as sweet, but a CR response may not offer the same benefit to all patients!
I am glad to report we are finally seeing this level of detail from a few of
the better designed clinical trials. We have reported in prior articles
the results of the RF (Rituxan + fludarabine) trial at Ohio State (see
Fludarabine Monotherapy Is No Longer
the Gold Standard).
This article reviews the latest results reported from OSU, in which overall survival and
progression free survival information is broken down in terms of risk
categories of patients that took part in their clinical trial.

To refresh your memory, this pivotal study of patients who underwent RF therapy had two arms to it. Roughly half of the patients had R and F concurrently, and the other half had the two drugs one after the other, that is, sequentially. After a couple of years, there was not much difference between the two groups (in other words, it did not matter much whether the patients got the R and F simultaneously or sequentially). The overall response rate for the whole group was an impressive 92%, and a hefty 43% of the patients got the coveted “CR”. Most studies end there, resting on their laurels of high overall response rate and high percent of CRs in this relatively high risk group of patients. I am delighted the researchers at Ohio State who conducted this trial went further, looking for overall survival and progression free survival statistics, and tried to determine whether patients in different risk buckets had the same bang for the buck. Their abstract is given below. If you would like to read the full text of the article, please write to us and we will help you locate it. If you are considering RF therapy as your next step, I suggest this is one article that you need to read carefully.
J Clin Oncol. 2026 Dec 12; [Epub ahead of print]
Select High-Risk Genetic Features Predict Earlier Progression Following Chemoimmunotherapy With Fludarabine and Rituximab in Chronic Lymphocytic Leukemia: Justification for Risk-Adapted Therapy.
Byrd JC, Gribben JG, Peterson BL, Grever MR, Lozanski G, Lucas DM, Lampson B, Larson RA, Caligiuri MA, Heerema NA.
Division of Hematology-Oncology, Departments of Internal Medicine and Pathology, The Ohio State University, Columbus, OH; Department of Medical Oncology, Dana-Farber Cancer Institute, Boston, MA; CALGB Statistical Center, Durham, NC; Department of Medicine, The University of Chicago, Chicago, IL.
PURPOSE: Several new prognostic factors predicting rapid disease progression
in chronic lymphocytic leukemia (CLL) have been identified, including
unmutated Ig VH mutational status, del(11)(q23), del(17)(p13.1), and p53
mutations. To date, the impact of these same prognostic factors have not
been examined relative to treatment outcome with chemoimmunotherapy.
METHODS: We examined the impact of these new prognostic factors on
predicting treatment outcome in symptomatic, untreated CLL patients who
received chemoimmunotherapy with fludarabine and rituximab as part of a
completed, randomized phase II study, Cancer and Leukemia Group B (CALGB)
9712.
RESULTS: Eighty-eight patients treated as part of CALGB 9712 had
detailed prognostic factor assessment performed. Using Ig VH mutational
status to classify risk, there was no association between complete response
rate with either unmutated Ig VH mutational status or high-risk interphase
cytogenetics. However, the median progression-free survival (PFS; P = .048)
and overall survival (OS; P = .01) were shorter among the Ig VH unmutated
patients as compared with the Ig VH mutated patients. Using the hierarchical
classification of Dohner, PFS (P = .005) and
OS (P = .004) were
significantly longer as the classification moved from high risk [del
(11)(q22.3) or del (17)(p13.1)] to low risk.
CONCLUSION: These data
demonstrate that high-risk CLL patients characterized by Ig VH unmutated
(>/= 98%) or high-risk interphase cytogenetics, including either del(17p) or
del(11q), appear to have a shorter PFS and OS with chemoimmunotherapy.
Larger prospective studies will be required to determine the independent
influence of Ig VH mutational status and interphase cytogenetics on
treatment outcome.
PMID: 16344317
____________
|
Patient Characteristics |
|
|
Total Number |
88 |
|
Median Age, Years |
63 |
|
Rai Stage |
|
|
Intermediate Risk |
64% |
|
High Risk |
36% |
|
IgVH Mutated |
32/75 |
|
IgVH Unmutated |
43/75 |
|
FISH Cytogenetics |
|
|
del(17p) |
3 |
|
del(11q) |
15 |
|
12Trisomy |
23 |
|
del(13q) |
24 |
|
Normal |
22 |
|
p53 mutated |
4 |
|
Abnormality |
del(17p) |
del(11q) |
12Trisomy |
del(13q) |
Normal |
|
Number of Patients |
3 |
15 |
23 |
24 |
22 |
|
% CR Response |
0% |
53% |
25% |
38% |
64% |
|
3-year Survival (%) |
33% |
53% |
74% |
75% |
86% |
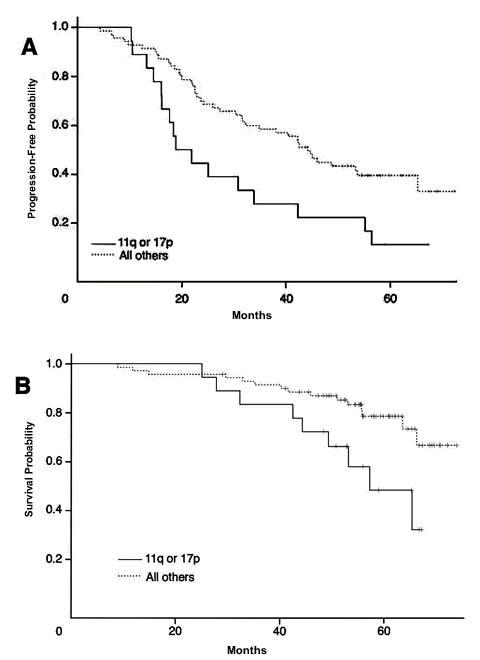
Now for the good stuff. Say we divvy up the patient cohort into two groups, those that had the dreaded 11q or 17p FISH deletions, and those that did not. Was there a difference between these two groups, in terms of how long the remissions lasted (i.e., there was no sign of CLL coming back), and even more important, was there any difference in how long they lived after completion of the RF therapy? Important stuff, right? The two graphs below (taken from the paper), show that there was a clear and significant difference between the two groups. Folks with 11q or 17p deletions relapsed sooner, and died sooner too. More than half of them relapsed in under 20 months, compared to roughly double that period for the group that did not have these poor risk FISH abnormalities. More than half of them were dead by the five year mark, while the group without 11q or 17p deletions is still trundling along. So, now, if you are thinking of indulging in RF therapy, would you say it is important to find out which group you belong to, before you sign up?
 |
|
FISH Category and Survival after RF Therapy |
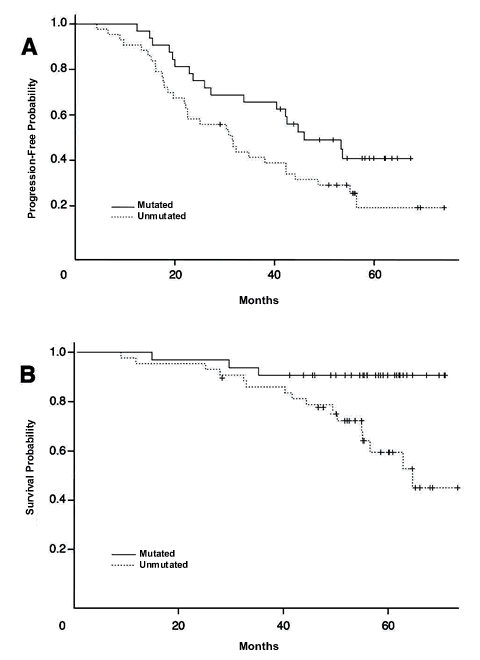
The pattern repeats all over again when the slicing and dicing is done in terms of another important prognostic indicator, whether or not the patients had the good mutated IgVH type or the more dangerous unmutated IgVH type of CLL. I think you can guess the answers by now, those with mutated IgVH type CLL had longer remissions free of CLL, and they lived longer too.
 |
|
IgVH Mutation Status and Survival after RF Therapy |
There is little question that combinations of Rituxan with chemotherapy drugs such as fludarabine will continue to be of use in treating CLL. But before you make therapy decisions it is important to know a little more than just the response statistics immediately after completion of therapy. This is particularly true for some of the more aggressive combinations, where more and more drugs are added on in an effort to goose the response statistics just a bit higher. As the guys who are on the pointy side of the infusion needle, you have to ask yourself whether the cost of the therapy is worth it to you. I am not talking about dollar cost, even though that too is important and especially so if you do not have medical insurance. Here I am talking about the health cost, the risk of immune suppression, opportunistic infections that can put you in the hospital, increased risk of secondary cancers such as basal cell carcinoma and squamous cell carcinoma that can be a lot more aggressive in CLL patients, cardiac and pulmonary toxicity, risk of transformation into more aggressive varieties of cancer such as the dreaded Richter’s transformation — the list goes on. We have discussed each of these at length in prior articles on Topics.
Unfortunately, even this paper does not address some of these issues. Were patients with poorer cytogenetics or unmutated IgVH genes CLL likely to have worse relapses, in the sense of relapsing with more refractory disease than they started out with? Were they hospitalized more often? Did they have a higher incidence of skin cancer and the like? I guess it will take larger studies and longer term monitoring to get these more fine-tuned details. But even as far as it goes, this paper is of tremendous value to patients and provides a model for trial design and reporting. The authors are pretty blunt in their own assessment. Below are some quotes from the paper, good advice to all patients as they consider therapy choices:
Bottom line, before you start RF therapy, it is important to find out your risk bucket. If you happen to have some of the more dangerous prognostics, you may want to re-think your strategy just a tad. I am willing to bet dollars to donuts the same logic would apply to other more elaborate chemo-immunotherapy combinations as well, such as FRC, FC, etc. As time goes by, we are hearing about increasing numbers of patients who are beginning to relapse, even if they achieved the coveted “pcr negative” remissions immediately after completion of RF or FRC therapies. Did these earlier relapsers have poorer prognostics going in, and did that override everything else, even if they had the same response classification getting out of the gate after completion of therapy?
Another important concept just got underlined for me unpleasantly a few days ago. I heard a good friend with solid pcr negative response after RF therapy has just relapsed. Here is the kicker: he has now relapsed with more refractory disease. He has a perfectly matched sibling, willing to be a stem cell donor. In hindsight, he wishes he had not wasted the clean remission he had 3 years ago. He now wishes he had gone straight from his pcr negative remission into a mini-allo transplant. Since he had a high-risk FISH mutation, it is now clear (in the perfect vision of hindsight) that his remission was going to be short-lived. Chances were higher that when he inevitably relapsed, he might have a harder time getting another such good remission. Mini-allo transplants have much better rate of success if done while the patient is in full remission, with just a trace of CLL remaining for the transplanted stem cells to deal with. Moral of the story — if your CLL is of the high risk variety and you are not likely to get too many really clean remissions, you might want to consider a stem cell transplant sooner rather than later.
It is also important to keep in mind that there are only so many bridges you can burn, only so many bullets available to you. Jumping the gun too soon because you are a type A personality and cannot deal with the daily hassles of CLL, or going for the most aggressive combination therapy you can find right off the bat because that will give you the best chance of a pcr negative CR (the best kind there is, right?), may not be a winning strategy for some patients. As in any other war, it is important to focus on the short term tactics, as well as the longer term winning strategy. As always, it is a matter of balancing the risks and rewards, and I will be the first one to admit that is easier said than done. Articles such as this one from OSU makes it just a bit easier to read the tea leaves. This paper is a refreshing change from other recent clinical trial reports that read more like marketing press releases than scholarly scientific publications written by medical professionals.
 Enter Keywords: |
———
Disclaimer: The content of this website is intended for information only and is NOT meant to be medical advice. Please be sure to consult and follow the advice of your doctors on all medical matters.
Copyright Notice:
Copyright © 2026-2007 CLL Topics, Inc. All Rights Reserved.
All materials contained on this site are protected by United States copyright law and may not be reproduced, distributed, transmitted, displayed, published or broadcast without the prior written permission of CLL Topics, Inc. You may not alter or remove any trademark, copyright or other notice from copies of the content.
However, you may download and print material from CLLTopics.org exclusively for your personal, noncommercial use.
———
